
There is a general practitioner shortage in Taree and it’s a crisis that is forcing medical centres to recruit overseas.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
It is transforming the face of general practice medicine in rural areas, it’s not isolated to Taree and Dr Simon Holliday of Albert Street and Harrington Medical centres says it is time the community learned why young doctors come and go so quickly from local medical centres and why the majority are overseas trained.
The Australian Government knows there is a problem with the recruitment and retention of GPs to the region as it recently relisted Taree to the Districts of Workforce Shortage (DWS) system.
The listing means Taree “is an area of Australia in which the population’s need for medical services has not been met”, according to the Department of Health.
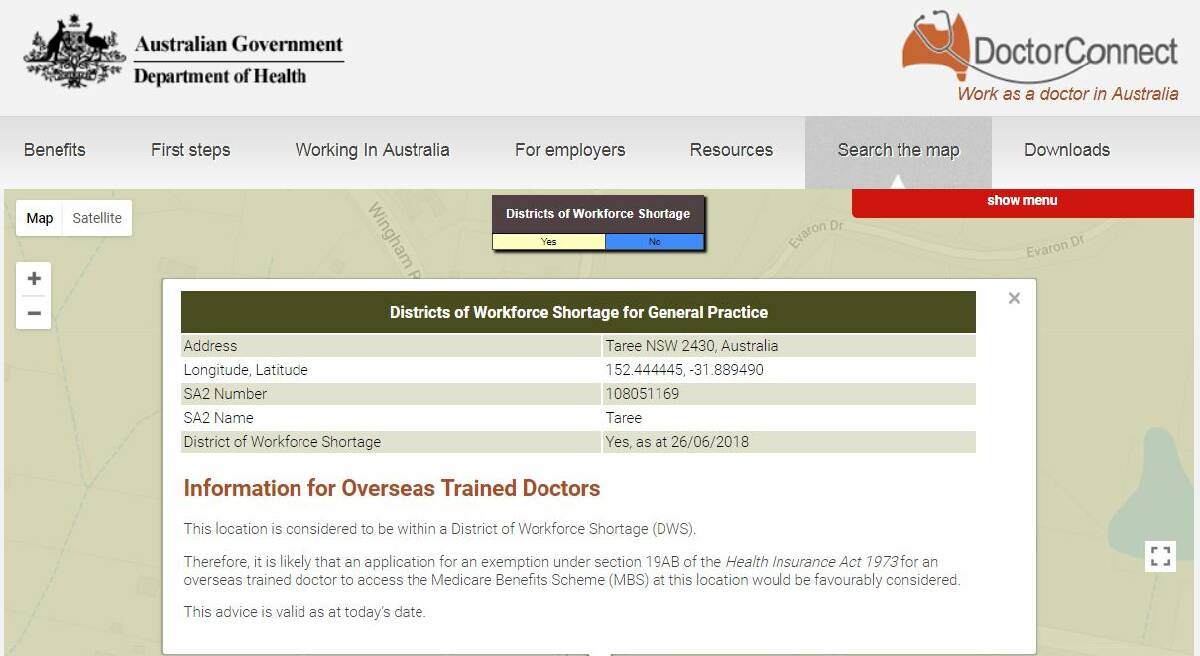
Taree is now listed with Harrington, Wingham, Old Bar, Nabiac, Gloucester and Bulahdelah. The DWS status opens the employment door to overseas trained doctors and foreign graduates of accredited medical schools and gives access to Medicare benefits for the services they provide.
The need to recruit overseas and the need for the DWS classification comes as Australian-trained GPs do not want to work in rural areas, according to Dr Holliday, and he says “there is nothing to compel them to do so.”
I’ve been shaking my fist at the sky for many years.
- Dr Simon Holliday
Dr Holliday stresses there is an increasing need for Australian-trained GPs in rural areas and says, “there is no actual system, just multiple bureaucratic barriers.”
He believes it is time the community gave voice to its dissatisfaction, to its concerns and he says it needs to be directed to State and federal politicians – and not to the “exhausted doctors in general practice because there is absolutely nothing more they can do.”
Dr Holliday operates two medical centres in the region, one in Taree and the second in Harrington, and he knows people are concerned about the high turnover of GPs because it is a constant theme of conversation.
“We get new people coming to our practice and they will say, ‘Every time I go to practice A, B or C they have a different doctor and I'm sick and tired of it. I'm now coming to you because you've been here for some time’. Sadly I have to say that I personally can't take any more patients, and that our practice, just like your previous practice, also suffers from a transient medical workforce problem.
People are wanting consistency of medical practitioner; they want a relationship with their doctor.
Dr Holliday hopes casting a spotlight on the problem and its causes will be a catalyst for community action that will compel Myall Lakes MP, Stephen Bromhead and Lyne MP, Dr David Gillespie to take the issues to government and “tackle institutional inertia and begin to do something.”
“I think the people have got to tell them, ‘We want better health services. Our society has organised education at universities and hospitals to be culturally appropriate and rural communities deserve the rewards of that training which our taxes have been funding. We want to have long term relationships with doctors so they can get to know us, so they can get to understand our problems and so we don't have to explain our problems to a new doctor every five minutes’,” Dr Holliday said.
The recent retirement of Dr Colin Rose OAM from Taree Medical Centre adds to the exodus of older Australian-trained GPs from the region, and Dr Holliday says “the only replacements are overseas trained doctors or junior doctors doing registrar training.”

“We rarely have locally-trained doctors even applying for jobs which aren't just temporary training positions. We need to change the system to reflect a social obligation for doctors who are trained in Australia to do time in the bush.”
Dr Holliday says rural-bonded scholarships from universities do not guarantee Australian-trained GPs will come to rural areas as “at least one third of them are breaking the contract and just not doing it. They'd rather pay the money back than do the time in the bush, so the politicians must set up a functional system.
“We wouldn't have a problem if rural service was mandatory for our graduates just as it is for overseas medical graduates. Creative approaches may include establishing incentives to go to the bush - it might be that your HECS fee is halved if you did time outside the cities.”
Dr Holliday says it’s time for State and federal governments to “look at what's going on at the coalface.” He acknowledges it is a complex issue and says it will involve conversations between several State and federal government departments.
He says he has been writing to, and meeting with, our local politicians for years. The lack of an easy or quick fix “does not mean they should do nothing.”
“We need to have the politicians and regulators talk to us. The system is broken. Right now each public servant in their silo does their own policies and procedures and no-one actually says, how do we make the system work effectively?”

Dr Holliday says the issue must not be kicked-off to a government committee process with any resulting report shelved. He says it’s time rural health, and this issue, is made a political priority.
“Rural Australia definitely has a far worse doctor-per-head-of-population ratio than the cities, and almost always we have worse measures of health outcomes than urban people. The reality is that many people can’t access continuity of care and quality care.
“If they are going to a practice where they have five-minute medicine, they (a GP) is racing through 12 people an hour and that's often not going to deliver quality care.

“If you are going to a patient-centred practice where they're going to spend more time with you and take a more wholistic approach to what is going on in your health and suffering, it's going to take more than five minutes. This means you may be waiting a lot longer to get in.”
Dr Holliday is thankful Taree practices can now access much-needed overseas trained doctors. However, this will not prevent the exodus of GPs who have completed their registrar training or, for overseas doctors, their compulsory rural service.
“They usually head straight back to the cities,” Dr Holliday said.
Access to elite schools, greater professional employment opportunities for their spouse, and connection with people from their own native language group are three reasons Dr Holliday gives for the exodus.
“Reform is needed. The health of our rural communities shouldn’t be sacrificed because of political ‘pass-the-parcel’.”
HAVE YOUR SAY:
Click here to do a multiple choice survey on the GP shortage.

